Reflux is no joke!
Many of us have regretted overeating late at night or drinking too much when it results in a night of belching, bloating and acid reflux. Long term this is no joke blokes, party goers, big eaters and those who are stressed!
Gastroesophageal reflux disease (GERD) influences patients’ general health, physical and emotional abilities and activities. Heartburn or reflux has many causes. From lifestyle habits to inadequate or too much hydrochloric acid (HCL) secreted in the stomach, to pregnancy and a host of other illnesses.
HCL is an essential acid that assists protein digestion, inhibits undesirable pathogens (bugs) in the stomach and protects the small intestine from bugs, yeasts and more. HCL encourages the flow of bile and pancreatic enzymes that assist the breakdown and ultimately the absorption of nutrients from our food including folate, vitamin B12, ascorbic acid, beta-carotene, iron, and some forms of calcium, magnesium, and zinc. Studies have shown that hydrochloric acid secretion from the stomach lining starts within hours after birth, peaking in our 30’s and declines with advancing age.
Overproduction of HCL is also of concern as it can create inflammation and ulceration of the stomach and oesophageal lining. This may be a result of medications (the body tries to compensate for the lack of HCL), stress and other imbalances and illness. The over use of antacids or acid blockers leading to low levels of hydrochloric acid can result in poor protein digestion, inflammatory bowel issues and reduced nutritional absorption.
Acid reflux (GERD or gastroesophageal reflux disease) occurs when stomach juices containing HCL and an enzyme called pepsin flows back up into the oesophagus – food pipe and up towards the mouth. If not corrected early reflux will likely create inflammation that damages the valve (sphincter). Named Erosive Esophagitis, (EE) is one of the most common complications of GERD and at its worst may result in cancer of the oesophagus.
The gastroesophageal sphincter is a muscle at the intersection of the oesophagus (esophagus – is the American spelling) to the stomach that normally acts as a valve letting food into the stomach when we eat then swallow food. Like other valves in our veins and heart they do not let fluids go backwards, until they cannot close off properly. When we vomit the valve is forced open! With continued stressful eating with or without vomiting and unhealthy lifestyle habits this valve may weaken and eventually fail. The stomach contents are regurgitated back into the oesophagus, creating symptoms of acid reflux (GERD). Acid reflux causes an internal burning sensation (heart burn), a sensation of something stuck or a sour taste in the back of the throat and oesophagus. It is now thought the certain coughs, sinus and dental issues are associated with indigestion and Gerd.
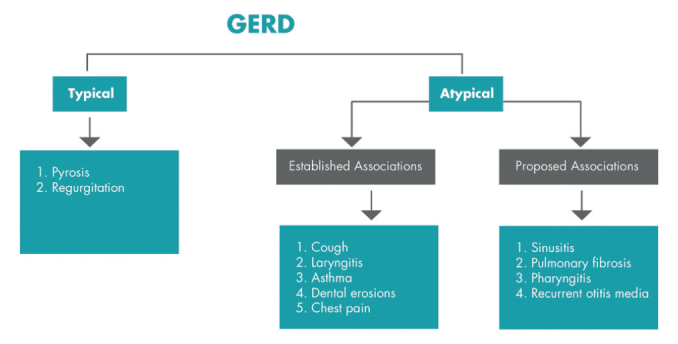
Highly processed fatty, salty and or spicy foods, grains and other foods (and other acidic foods like orange juice, tomato sauce, coffee chocolate, peppermint! and more) may aggravate acid reflux. Other factors that can cause or increase reflux include being overweight, smoking, alcohol, eating disorders, bulimia, stress and anxiety. Eating fast, on the go and large meals anytime or close to bedtime make reflux much worse. The use of non-steroidal anti-inflammatory drugs, some medications and pregnancy and lower levels of HCL and Pepsin enzymes) are other causes. Unfortunately oesophageal or gastric surgery and simply getting older can be other causes.
Occasional episodes may be relieved with over the counter antacids to reduce the acidity of the stomach. However these medications do not repair the inflammation to the valve, oesophagus or deal with the underlying causes. Long term frequent use of antacids can have harmful side effects: constipation, diarrhoea and food sensitivity and nutritional deficiencies (anaemia). Antacids (some contain aluminium) may also cause calcium loss which is not good for our bones and may lead to osteoporosis.
Stress is another significant cause of reflux. “ Anxiety and depression were significantly higher in patients with GERD, particularly those who also reported concerns of chest pain. Measures should be taken to reduce the stress and anxiety of GERD patients to cope with their daily life activities and improve their quality of life”. Stress appears to relax the sphincter and increase production of HCL.
What can we do to reduce indigestion and reflux ?
Lifestyle comes first – It’s often all up to us!
- Eat a little, sit up a little longer! Eat healthy food slowly in smaller amounts with occasional treats.
- Let your body digest your food for two to three hours before lying down. HCL is generated within one hour of eating so it is very good to be up and about after a meal
- Do not wear clothing that constricts the abdomen. Added upward pressure on the stomach may cause acid to back up into the oesophagus
- Get on to programme to reduce weight if needed
- Keep a food journal to understand the foods eaten and time of day symptoms arise. This includes alcohol!
- Do not eat close to exercise or heavy lifting
- Find solutions to reduce stress
- Reduce coffee, alcohol and unnecessary medications if life style modifications and herbal medicines can be used as the first option.
For those with chronic daily indigestion and reflux it’s a more complex management programme
Our digestive enzymes break down our food really well so that we can absorb lots of wonderful nutrition to keep us strong and healthy. Therefore any suppression of our digestive process can have quite an effect on our health in the long term. The natural health perspective on wellness starts with a healthy digestion and therefore lifestyle habits.
The following information is for those that really do have problems that are not sorted by eating healthy food at the right times of the day, not night!
For those taking common medications for GERD or Reflux (such as PPI’s, Omiperazole) we can suggest various herbs and supplements to work alongside your medications and help to repair inflammation in the oesophagus or stomach (gastritis). No one should abruptly change their medications and we strongly recommend that you completely understand the actions and long term issues that may be associated with medications, natural digestive aides and not embracing a healthy eating style.
Herbs and Supplements
Thankfully there are specifically designed natural remedies for reflux using herbs and nutrients to provide rapid support for indigestion, heartburn, acid reflux, and an upset or a sour stomach. And unlike some over the counter medications, no aluminium or other harmful ingredients.
Hoheria, Marshmallow root and Slippery Elm bark all contain polysaccharides providing mucilaginous properties to soothe inflamed linings of the digestive tract while ginger root, papaya fruit and liquorice root work together to aid digestion. Dandelion and Gentian also help to aid your digestion and breakdown of your food.
Melissa, Valerian, St Johns Wort, Kawakawa, Chamomile and Saffron are all possible inclusions in a herbal tonic to reduce the effects of stress. Pregnant women can use herbal medicine with supervision by a herbalist or naturopath.
Natural remedies for acid reflux can create a buffer, reduce acidity of the stomach acid (a little) and help support the lining of the gastroesophageal sphincter and oesophagus.
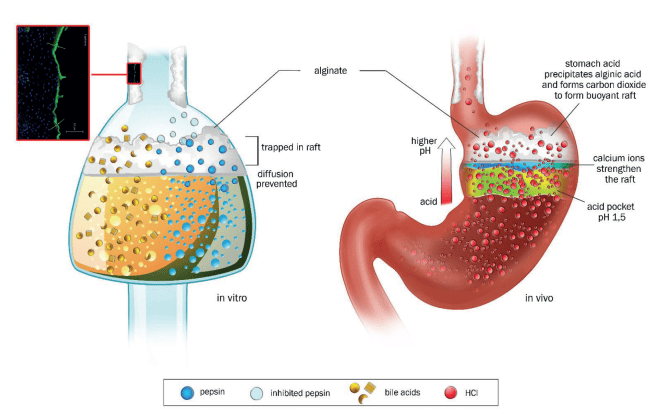
Calcium carbonate – for serious indigestion and in small amounts – helps buffer acidity and Alginic acid (which converts to sodium alginate) helps to maintain the mucous lining of the oesophagus.
Sodium alginate is a natural polysaccharide extracted from brown algae – brown seaweed (Laminaria hyperborea). Sodium alginate is effective for suppressing reflux. Alginates may be a good alternative to PPIs for on-demand treatment from babies to pregnancy and adults.
How do alginates work?
It takes several hours to raise the intragastric pH above 4 after the first dose of PPIs (85), while Alginates have a unique mode of action that provide quick relief.
When sodium alginate mixes with the acid in your stomach, it forms a “raft” that floats on the top of your stomach contents. This creates a physical barrier over your stomach contents, which stops the excess stomach fluids containing acid coming back up into your oesophagus (food pipe) – helping to soothe symptoms of reflux and indigestion.
Caution: Calcium carbonate is known to effect the absorption of some medications. You should take other medicines one hour before or at least four hours after taking any antacid to prevent interactions. Also get advice if you have kidney and cardiac problems, have osteoporosis or are on any medications.
Treatment with an alginate product may reduce other digestive acids of pepsin and bile in your stomach contents that can contribute to reflux symptom. Therefore addressing the cause is the first priority and take only if needed!
Can I take an antacid if I’m pregnant or thinking of becoming pregnant?
Heartburn in pregnancy is common and it’s usually safe to take reflux and indigestion remedies while pregnant. Acid reflux in pregnancy is due to the hormone progesterone that relaxes joints and sphincters in the body, including the sphincter between the oesophagus and stomach. The pressure on the stomach due to the enlarging uterus. Both factors resulting in reflux!
Thankfully taking natural antacids short term during pregnancy, while you pay attention to what and when you eat can greatly improve quality of life for a pregnant mum. Alginates are safe and very useful, act quickly and can be used as an on-demand therapy. It is also important to check the ingredients and don’t take more than the daily recommended dosage. For those less fortunate, the nausea and reflux symptoms do not finish at the end of the first trimester and may be far more serious. Always check in with your midwife and GP.
So If you have read all the way to the end of this post and have any questions please get in touch
This article is in not prescriptive as each person will have requirements unique to their health condition. Consult your healthcare professional or Bodywise to see what we can suggest for your reflux and any associated health concerns.
You might also like to read
Vitamin D for mothers and babies and everyone else
Taurine – the established benefits for energy, repair and mood
Time for a spring clean and detox
